 
For that reason, it is recommended to switch from AAIR to DDDR in these cases. This seems not to be a real physiological pacing mode because of the possible consequences of such a long AV interval in the LV filling pattern. Since there is no limit for the AV interval in the MVP algorithm, it is possible to see patients with first degree AV block, long AV interval (400 ms in our case), and an AAIR operation. This allows fast switch to DDD(R) mode but does not cause false switching on a single non-conducted atrial event. The criterion to switch is loss of AV conduction for two out of the last four pacing cycles (the four most recent A–A intervals). MVP switches from AAI(R) operation to DDD(R) operation when there is evidence of persistent loss of AV conduction. After a first A–A interval with no conducted VS, a backup VP is delivered 80 ms after the AP stimuli ( Figure 2 ). The algorithm allows prolonged AV intervals and occasional, single, non-conducted normal atrial contractions (sensed or paced). 
It is an atrial-based pacing mode that looks for any consecutive A–A intervals without associated ventricular events. MVP algorithm is designed to avoid unnecessary VP preserving intrinsic conduction. device with MVP (managed ventricular pacing) algorithm and the pacemaker had an adequate functioning. The patient had received a Medtronic Inc. Then, an atrial stimulus followed by a ventricular paced event with a very short AV interval can be seen reinitiating the Wenckebach phenomenon ( Figure 2 ). The second ECG shows again atrial pacing at 70 bpm with a progressive prolongation of AV interval and intrinsic ventricular events until one of the atrial stimulus is not conducted to the ventricle, that is, a 4:3 Wenckebach phenomenon. There is no switch from AAI(R) operation to DDD(R) operation since there is no loss of atrioventricular conduction for two out of the last four pacing cycles. Atrial pacing at 70 bpm and a 4:3 Wenckebach phenomenon initiating managed ventricular pacing algorithm. A second ECG performed a few minutes after initial evaluation gave us the answer ( Figure 2 ). At this point, differential diagnosis includes: (i) inadvertent programming to AAI(R) mode (ii) crosstalk (iii) an inaccurate AV interval programming which seems improbably because the estimated AVI is near 400 ms and (iv) finally, it could be a case of a pacemaker pseudodysfunction, that is, a misinterpretation of normal function. The atrioventricular (AV) interval is prolonged. The 12-lead ECG shows pacing stimuli at 70 beats per minute which seems to capture in the atrium followed by a regular intrinsic ventricular response at 70 bpm. The atrioventricular interval is near 400 ms. 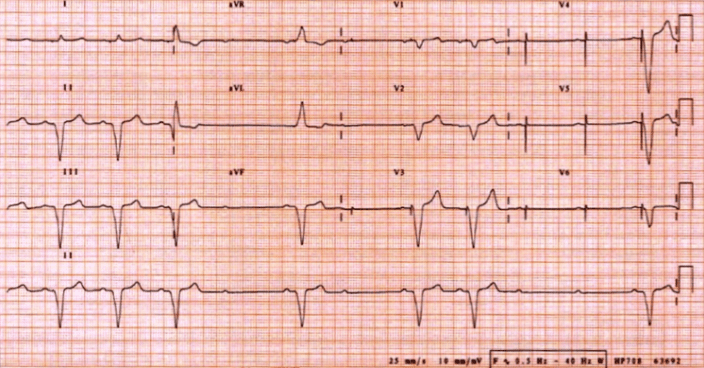
Pacing stimuli at 70 beats per minute capturing in the atrium followed by a regular intrinsic ventricular response at 70 bpm. Twelve-lead ECG obtained after initial evaluation. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
